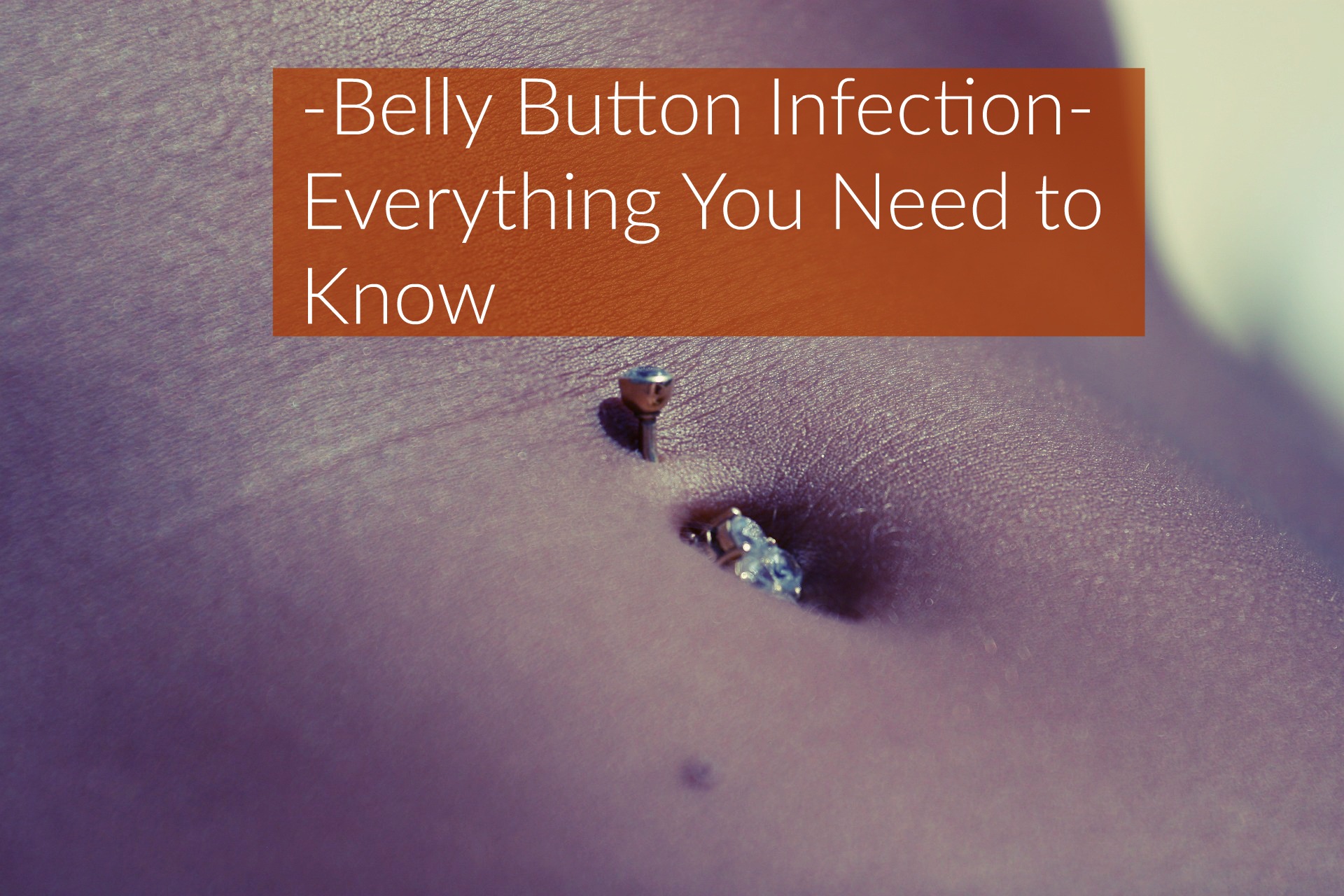
According to a 2012 research published in the journal PLOS ONE, more than 2,300 species of bacteria cover the belly button.(1)
In healthy individuals, these bacteria can’t cause problems…
A few risk factors and lifestyle choices (piercing :)), however, could contribute to an increased risk of a belly button infection.
Infections in the belly button, whether bacterial or caused by yeast overgrowth, are a relatively common problem.
It’s easy to see that something has gone terribly wrong. Discharge and an odd odor are usually indicative of an infectious process.
The shape of the belly button contributes to an increased risk of infections, especially if hygiene has been compromised.
Are you worried that you may be experiencing a belly button infection?
Here’s how to tell what’s going on and how to decide whether medical assistance is required.
What is a Belly Button Infection?
The belly button (navel or umbilicus) is a natural bodily cavity that gives bacteria and yeast everything that they need to grow.
It’s warm and damp, various substances and sweat residue can easily build up inside.
This is precisely what infection-causing bacteria need to grow and form a colony.
Types of Infections
There are several types of infections in belly button:
Bacterial infection: as already mentioned, bacteria are the most common culprit.
All kinds of substances (sweat, lint, residues of cosmetic products) give the bacteria “food” for growth.
Brown or yellow belly button discharge is a common symptom of a bacterial problem.
Sebaceous cysts: a sebaceous cyst forming in the belly button region could also contribute to infection, pain or swelling.
If the cyst gets scratched excessively, it could easily get infected.
Fungal infections: candida is the most common cause of a fungal infection. It can affect any part of the body, including the navel.
Red and tender belly button that’s surrounded by flaky skin is most commonly indicative of a candida problem.
Urachal cysts: the urachus is the duct located within the umbilical cord that enables the drainage of urine from the bladder of the fetus.
It’s rarely possible for the duct to remain open in kids and adults.
The infection of this canal is called urachal cyst and it will have symptoms similar to those of the typical infection.
Diabetic infection: people that suffer from diabetes are more prone to experiencing naval infections than healthy individuals.
A cottage cheese-like discharge is typical for the belly button infections caused by diabetes.
 Causes and Risk Factors
Causes and Risk Factors
Several factors could contribute to frequent infections in a belly button.
A few behaviors may aggravate the condition and slow down the healing process.
Infected Belly Button Piercing
According to the Statistic Brain Research Institute 2015 research, Naval is the most popular piercing location for women. The research also showed that 31 percent of body piercing’s had complications.
People that have belly button piercings are more prone to experiencing such infections than other individuals.
The risk is high if hygienic procedures aren’t followed strictly during the piercing process, according to the NSW Ministry of Health.
In essence, the piercing creates an open wound. Until it heals, the wound can harbor all kinds of bacteria and get infected easily.
Hygiene
The second risk factor is poor personal hygiene. Infrequent bathing keeps substances and sweat buildup inside the belly button.
Bacteria and fungi start to grow. The process is accelerated and the overgrowth leads to an infection.
The bathing technique is also important. Soap and water that remain inside the belly button are quite harmful.
People that don’t have access to clean water for bathing are also susceptible.
Though these are the main risk factors, a few others will also have to be mentioned:
» Frequent touching of the belly button: many species of bacteria can survive on the fingertips.(2)
People that habitually touch the belly button or that play with a piercing are at a higher risk of experiencing a belly button infection.
» Recent abdominal surgery: statistics suggest that a recent surgery can contribute to a higher risk of infection.(3, 4)
» Obesity: being overweight or obese created excellent conditions for the growth of bacteria and fungi.(5,6)
People who are morbidly obese may also find it difficult to maintain proper personal hygiene and clean all of the bodily crevices or folds thoroughly.
» A cut or a wound: a cut on any part of the body that’s not treated and disinfected can easily become red and swollen.
» Clothing choices: tight fitting clothes, elastic bands and synthetic fabrics don’t cause a belly button infection but they can aggravate the symptoms.
An elastic band that rubs harshly against the belly button may wound the region or cause you to scratch your belly.
Synthetic fibers don’t absorb moisture, which creates the perfect conditions for the growth of bacteria and fungi.
» Pregnancy: just like tight clothing, pregnancy does not cause belly button infections. It does, however, increase the risk.
Most women experience mild belly button pain during pregnancy because of the stretching.
If redness, tenderness and discharge also occur, ladies will need to see a physician.
The Diagnostic Process
The most common symptoms of belly button infection that people experience include the following:(7, 8, 9)
» Pain, swelling and redness in the belly button region
» Excessive skin warmth
» A constant itch or a “tingling” sensation
» The discharge of pus, a greenish, yellow or brownish liquid
» Bad odor
» Bleeding from the belly button
» Vomiting and dizziness (this is only in severe cases)
There are several conditions that could cause those symptoms apart from a navel infection.
This is why you have to see a doctor as soon as you experience something unusual.
Skin conditions like psoriasis could cause symptoms that are similar to those of an infection.
Some rare forms of cancer may also express themselves in similar ways.
A physical exam will usually be sufficient to diagnose a belly button infection.
In some instances, a physician may want to have a couple of lab exams to rule out other causes.
A swab will also be taken to the lab to identify the types of bacteria or fungi that are leading to the infection.
Best Treatments for Belly Button Infections
Two categories of treatments exist – some of them are prescribed by a physician, others are DIY solutions.
Before attempting to treat a belly button infection on your own, you may want to have a consultation with your physician.
Medical Treatments
 Most people see their doctor while the infectious process is still mild.
Most people see their doctor while the infectious process is still mild.
In such instances, topical antibiotic ointments like Neosporin, Polysporin First Aid Antibiotic or Duospore, will be sufficient to kill the bacteria and resolve the issue.
Doctors will also prescribe antibiotics alongside the topical treatment for more serious infections.
The course of treatment will usually continue a couple of days.
Surgery is required solely in extreme cases of belly button infections.
This is why it’s imperative to seek medical assistance as soon as the first strange symptoms are experienced!
Physicians may also recommend salt water rinses to destroy the bacteria.
The rinse is made by dissolving a teaspoon of salt in warm water. Saline solutions are also available in most pharmacies.
After the belly button has been rinsed, it should be dried thoroughly with a soft towel.
People that have a piercing will need to remove it until the infection subsides.
Discharge can be cleaned with hydrogen peroxide (a mild antiseptic) to keep the area dry and clean.
Popular Home Remedies for Belly Button Infection
A couple of home remedies can be used for the effective management of belly button infections.
The aim of most treatments is to kill the bacteria or control the candida overgrowth.
Tea Tree Oil
Tea tree oil is one of the most popular natural treatments for infection in the belly button.
According to a report published in the Clinical Microbiology Reviews journal, it has powerful antibacterial, antimicrobial and antiseptic properties.(10)
Tea tree oil can be diluted in coconut oil and applied to the affected region several times per day. Don’t apply undiluted tea tree oil to the navel region. (check price on amazon.com)
Turmeric (Curcuma longa) Powder
Turmeric is also known for its powerful antibacterial and antifungal properties.
In fact, according to a 2015 study published in the European Journal of Pharmacology, Curcumin (the primary polyphenol in turmeric) may have “anticancer and antifungal effects in cancer and associated complications from invasive fungal infections.” (11)
Add a little bit of water to your turmeric powder and stir.
You should get a thick paste. Apply to the inflamed region and let it dry. After the turmeric powder dries completely, clean the area gently and pat it dry. (check price on amazon.com)
The symptoms of infection can disappear in a couple of days.
Rating | Product | Our Rating | Price on Amazon |
|---|---|---|---|
#1 | |||
#2 | |||
#3 | |||
#4 | |||
#5 |
A few other home remedies that you should consider include:
Neem (Indian lilac)
According to the Infinity Foundation ( D.P. Agrawal), neem cleanses the skin and kills harmful bacteria.(12) You can make a paste from the neem leaves. (check price on amazon.com)
Neem powders and creams are also available in cosmetic stores and online. Neem powder can be mixed with turmeric to deliver even better results.
White Vinegar
You might not know it but you’ve probably got a multi-purpose health product sitting in your kitchen… Vinegar can kill many types of bacteria, according to a study published in the Infection Control and Hospital Epidemiology, so this treatment could be beneficial in the case of belly button infections caused by bacterial infection.(13)
You will need to dilute one part of white vinegar in two parts of lukewarm water. Soak a cotton swab and apply to the belly button area.
Let the compress act for 10 to 15 minutes, remove the cotton ball and dry the skin. The procedures can be repeated two to three times per day.
Aloe Vera
aloe vera juice has soothing properties. The beneficial plant is also known to kill harmful bacteria, according to a 2013 report published in the Organic and Medicinal Chemistry Letters.(14)
For best results, you should use fresh aloe vera juice (obtained straight from the plant). Just cut a leaf open and apply the juicy part to the infected skin. (check price on amazon.com)
Leave it on for a few minutes and clean the area. The aloe vera juice should reduce the inflammation and it will also provide almost immediate symptom relief.
Calendula
Originally grown in the Mediterranean region, whilst adding color to the garden was revered for its wonderful powers of healing…
Calendula is a soothing herb that has anti-inflammatory properties, according to a 2009 study published in the Indian journal of experimental biology.(15) It’s great for managing the symptoms of a belly button infection.
Make some calendula tea, soak a cotton ball in the lukewarm liquid and apply to the belly button region. Keep the compress on for 10 to 15 minutes. (check price on amazon.com)
Apply frequently, especially if you’re finding it difficult to cope with the infection symptoms.
Coconut Oil
Coconut oil is a good energy source but also contains antifungal and antimicrobial ingredients.(16,17) It kills the bacteria and slows down the growth of fungi that cause infections.
The Department of Medical Microbiology & Parasitology from Nigeria concludes that “Coconut oil should be used in the treatment of fungal infections”.(17)
Coconut oil will also reduce the redness, pain and skin hotness linked to belly button infections. (check price on amazon.com)
Bear in Mind
If you don’t experience improvement within a day or two of starting the DIY treatment, see your physician.
You should also see a doctor if the infection symptoms become worse or you experience sharp belly button pain.
Resolving the issue in a natural way is highly desirable but you could be jeopardizing your health by postponing a traditional pharmaceutical treatment.
Prevention and Reducing the Risk of Infections
If you’ve just had a piercing, you suffer from diabetes or you’re at any other risk of experiencing a belly button infection, you should consider preventative practices:
» Always wash your hands with soap thoroughly or use the alcohol hand rub before handling the piercing you’ve just gotten. Hand washing removes germs and helps prevent infections.(18)
» Don’t play with it and don’t pull on it.
» Try not to sleep on your stomach.
» Rinsing the area with a saline solution (even when you’re healthy) will be great to prevent bacterial overgrowth.
» Change your clothing choices. Opt for loose garments made of natural fabrics like cotton and linen. They will keep your skin dry and reduce the risk of irritation.
» Have a shower once per day and use soap to gently clean your entire body.
» Rinse your skin with water and make sure that no traces of soap or shower gel are left behind. Pat yourself with a towel after coming out of the shower.
Make sure that every crevice is dry before getting clothes. Using the towel on your skin is a nice form of massage that can improve circulation – dedicate a couple of minutes to the activity.
» If you’re prone to experiencing candida issues, you may want to consider a change in diet. Reduce the intake of sugary and processed foods, alcohol, peanuts…(19)
» Don’t use public swimming pools after getting your belly button pierced
» Eat more raw fruits and veggies. Junk food does taste delicious but it makes your body susceptible to a wide array of problems. With time, you’ll learn to enjoy whole and natural foods.
Effective prevention should be a priority. Plus, you’ll get to feel a lot healthier – who doesn’t want that?
Conclusion
Belly button infection can occur, even if you take perfect care of your body.
Remember that the sooner you address a medical problem, the easier it’s going to be to treat.
Don’t hesitate to contact your doctor right away, even if the symptoms are solely mild.
References
1.Hulcr J, Latimer AM, Henley JB, Rountree NR, Fierer N, et al. (2012) A Jungle in There: Bacteria in Belly Buttons are Highly Diverse, but Predictable. PLOS ONE 7(11): e47712. https://doi.org/10.1371/journal.pone.0047712
2.Edited by Chao-Lin Chen, Demosthenes Morales, Huynh Nga Vo, students of Rachel Larsen Human Hands and Fingernails 20 August 2010
3.Reichman DE, Greenberg JA. Reducing Surgical Site Infections: A Review. Reviews in Obstetrics and Gynecology. 2009;2(4):212-221.
4.Kiernan M (2012) Reducing the risk of surgical site infection. Nursing Times; 108: 27, 12-14.
5.skinsight.com: Skin Problems Related to Obesity Accessed 20 December 2017.
6.DR. TOM IAROCCI Skin Problems Related to Obesity Last Updated: Aug 14, 2017
7.Common Skin Infections Nathaniel C. Cevasco Kenneth J. Tomecki Published: August 2010
8.RICHARD P. USATINE, MD, and MARCELA RIOJAS, MD, University of Texas Health Science Center, San Antonio, Texas Am Fam Physician. 2010 Aug 1;82(3):249-255.
9.Candidiasis (Mucocutaneous) (Moniliasis) By Denise M. Aaron, MD, Assistant Professor of Surgery; Staff Physician, Dartmouth-Hitchcock Medical Center; Veterans Administration Medical Center, White River Junction Accessed 20 January 2018.
10.Carson CF, Hammer KA, Riley TV. Melaleuca alternifolia (Tea Tree) Oil: a Review of Antimicrobial and Other Medicinal Properties. Clinical Microbiology Reviews. 2006;19(1):50-62. doi:10.1128/CMR.19.1.50-62.2006.
11.Curcumin and its promise as an anticancer drug: An analysis of its anticancer and antifungal effects in cancer and associated complications from invasive fungal infections Authors Jin Chena Zheng-Min Hea Feng-Ling Wanga Zheng-Sheng Zhanga Xiu-zhen Liua Dan-Dan Zhaia Wei-Dong Chenb https://doi.org/10.1016/j.ejphar.2015.12.038
12.Medicinal properties of Neem: New Findings by D.P. Agrawal Accessed 19 February 2018.
13.Rutala, W., Barbee, S., Aguiar, N., Sobsey, M., & Weber, D. (2000). Antimicrobial Activity of Home Disinfectants and Natural Products Against Potential Human Pathogens. Infection Control & Hospital Epidemiology, 21(1), 33-38. doi:10.1086/501694
14.Nejatzadeh-Barandozi F. Antibacterial activities and antioxidant capacity of Aloe vera. Organic and Medicinal Chemistry Letters. 2013;3:5. doi:10.1186/2191-2858-3-5.
15.Kuttan, G., Kuttan, R., & Preethi, K.C. (2009). Anti-inflammatory activity of flower extract of Calendula officinalis Linn. and its possible mechanism of action. Indian journal of experimental biology, 47 2, 113-20.
16.Novel Antibacterial and Emollient Effects of Coconut and Virgin Olive Oils in Adult Atopic Dermatitis Authors Vermén M. Verallo-Rowell, Kristine M. Dillague, Bertha S. Syah-Tjundawan, Skin and Cancer Foundation, Pasig, Philippines, and the VMV Skin Research Centre + Clinics, Makati City, Philippines Dermatitis. 2008;19(6):308-315. © 2008 American Contact Dermatitis Society
17.D.O. Ogbolu, A.A. Oni, O.A. Daini, and A.P. Oloko. Journal of Medicinal Food. December 2009, 10(2): 384-387. https://doi.org/10.1089/jmf.2006.1209
18.Show Me the Science – Why Wash Your Hands? Content source: Centers for Disease Control and Prevention last updated: November 18, 2015
19.Dr. Axe. Candida Diet: The Foods & Supplements to Eat (and Avoid) to Treat Candida Accessed 18 February 2018.
Leave Feedback: Was this article helpful?